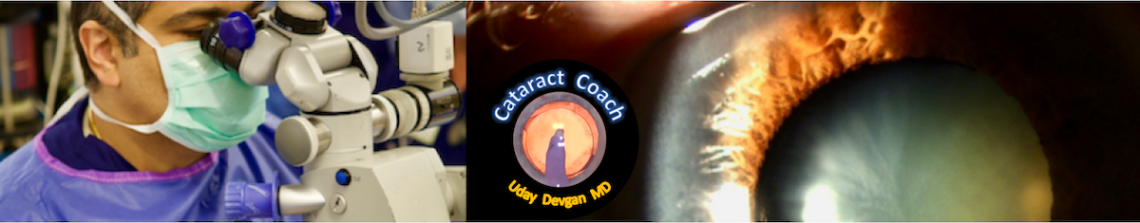
Stop reading and look carefully at the title picture here. What does this tell you? Seriously, stop reading and study the photo and ask yourself what is going on.
While most patients undergoing cataract surgery have good support of the lens capsule, there are cases in which zonulopathy can pose a challenge intra-operatively. Certain conditions such as pseudoexfoliation are associated with global zonular weakness, while ocular trauma is typically linked with focal or quadrant zonular loss. In many cases of focal zonular loss, the lack of capsular support is only noticed intra-operatively when the nucleus has been removed and the capsular bag is now unsupported by it.
The capsular equator sign
Unbeknownst to the surgeon, this patient sustained a car airbag injury many years before cataract surgery, but he failed to mention it at the consultation. The beginning of the surgery is uneventful with a normal capsulorrhexis and routine nucleus removal using the chop technique. Once the phaco probe is withdrawn from the eye, the capsular bag deflated, and the equator of the capsular bag is visible for about 2 clock hours (Figure 1). This critical sign is immediately recognized, and care is taken to avoid further complications. During a routine cataract surgery with good zonular support, the capsular bag equator should not be visible.

Remove cortex while supporting the capsular bag
As soon as this is noted, the circulating nurse is asked to open a capsular tension ring (CTR), which will be implanted to aid in capsular support. However, first we wanted to remove as much of the lens cortex as possible, starting with the areas of good zonular support. For most of the cortex, the zonular support of the capsule provides counter-traction to allow the cortex to be stripped away using the irrigation/aspiration (I/A) probe. For the last bit of cortex that is in the area of compromised zonular support, a second instrument such as a spatula is used to hold the capsular bag at the capsulorrhexis while the I/A probe removes the cortex (Figure 2). This additional support from the spatula helps to remove the cortex while preventing further zonular loss. Once the cortex is removed, it is important to fill the capsular bag with cohesive viscoelastic while keeping the anterior chamber pressurized to prevent vitreous prolapse.

Implanting the CTR
Because the area of zonular loss is about one quadrant (2 to 3 clock hours), placing a CTR is sufficient to provide robust capsular support. The capsular bag has a diameter of about 9 mm to 10 mm while CTRs are usually 11 mm to 12 mm in diameter. This allows the flexible CTR to exert an outward force at the lens capsular bag equator, distributing the forces equally and providing stability. To insert the CTR, care must be taken to avoid damaging the capsular bag. My preferred technique is to engage the leading eyelet of the CTR with a hook while it is delivered into the capsular bag (Figure 3). Then both eyelets are released, and the CTR is securely in position.

Implanting the IOL and finishing the case
With a supported capsular bag, just about any IOL will do well in this case, even presbyopia-correcting designs that require precise centration for optimal performance. In our case, the patient has chosen a monofocal IOL and a goal of plano, so a single-piece acrylic IOL is placed in the capsular bag. The lens is well supported and stays centered with the capsulorrhexis overlapping the optic securely (Figure 4).

As the viscoelastic is removed from the eye, the fluidic parameters are adjusted to give lower flow so as to not cause turbulence in the anterior chamber. A few tiny fragments of lens material may be present at the anterior hyaloid, behind the posterior capsule. During phaco, these pulverized lens bits can go through the area of zonular loss and rest on the anterior vitreous face. These will dissolve in the inflammatory cascade during the postop period and rarely pose a concern. There may be prolonged inflammation, which can be treated with additional corticosteroids. To ensure that no vitreous has prolapsed through the area of zonular loss, diluted intracameral triamcinolone can be injected into the anterior chamber because it will adhere to any vitreous strands. Patients with focal zonular loss from trauma present challenges during cataract surgery. With early detection of this condition and use of the aforementioned techniques, we can successfully complete these cases and provide the patients with excellent vision.